Imaging tests are an important step in figuring out whether a person has lung cancer. Imaging tests create pictures of the inside of the body by using X-rays, magnetic fields, sound waves, or radioactive particles.
Imaging tests cannot confirm that a person has lung cancer. However, they provide a lot of information to help put the whole picture together for the doctor. Imaging tests may be done before a diagnosis of lung cancer, during treatment for lung cancer, and after treatment. They are done for a number of reasons, including:
- To get more specific information about a suspicious area that might be cancerous
- To determine how far cancer may have spread
- To find out if treatment has been effective
- To monitor for possible signs of cancer coming back after treatment1,2
Different imaging tests a person might undergo include chest X-ray, CT (computed tomography or CAT) scan, MRI (magnetic resonance imaging) scan, PET (positron emission tomography) scan, and bone scan. These are explained below.
Chest X-ray
An X-ray is a type of high-energy radiation that goes through the body and onto film to produce a picture. A chest X-ray produces pictures of the bones in the chest and spine and the organs in the chest, including the lungs, airways, heart, and blood vessels.3,4
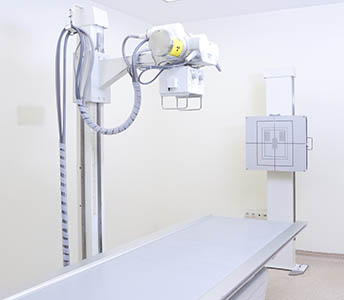
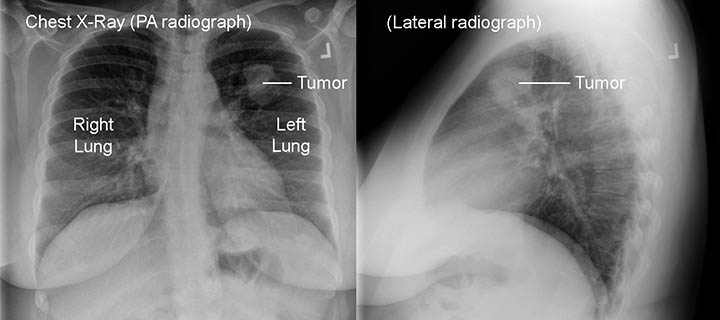
A chest X-ray is often the first test a doctor uses to look for a mass when symptoms are more general. However, chest X-rays often miss small lung cancers when the disease is in its early stage.2,5If you are concerned that you might have lung cancer, ask your doctor for a CT scan instead of, or in addition to, a chest X-ray.
Computed tomography (CT or CAT scan)
Computed tomography uses a computer linked to an X-ray machine to make detailed pictures of the inside of the body. Unlike a conventional X-ray, which takes one picture, a CT scanner takes multiple pictures as it rotates around the patient, in order to get images from different angles. Three-dimensional (3D) views of the organs and tissues can be created.
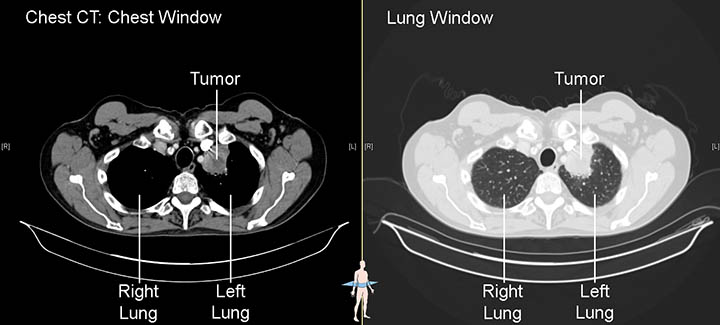
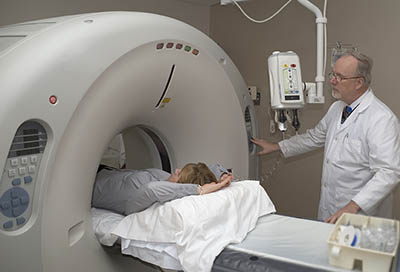 A CT scan can provide specific information about the size, shape, and position of masses or nodulesA growth or lump that may be malignant (cancer) or benign in the lung. It also can help find enlarged lymph nodes or masses in other organs that might be caused by the spread of lung cancer. It is important to note that, while a CT scan is very good at showing that something is there, it cannot tell what it is. For that, other tests are needed.6,7
A CT scan can provide specific information about the size, shape, and position of masses or nodulesA growth or lump that may be malignant (cancer) or benign in the lung. It also can help find enlarged lymph nodes or masses in other organs that might be caused by the spread of lung cancer. It is important to note that, while a CT scan is very good at showing that something is there, it cannot tell what it is. For that, other tests are needed.6,7
Sometimes a patient will be asked to drink a contrastA dye or other substance that helps show abnormal areas inside the body solution, or a dye will be injected intravenouslyInto or within a vein before a CT scan, so that some organs and blood vessels show up more clearly. A patient must not move while the pictures are being taken. Sometimes a patient may be asked to hold his or her breath for a few seconds. CT scans usually only take a few minutes to complete.6,7,8,9
Today, a low-dose CT scan (LDCT)A newer form of CT scan that uses less radiation than a standard chest CT and takes less than one minute to complete. It continuously rotates in a spiral motion and takes several three-dimensional, very detailed X-rays of the lungs. is most commonly used to look for lung cancer and follow up on changes in lung nodules. The radiation dose of LDCT is five times lower than that of a regular CT scan.9
Magnetic resonance imaging (MRI)
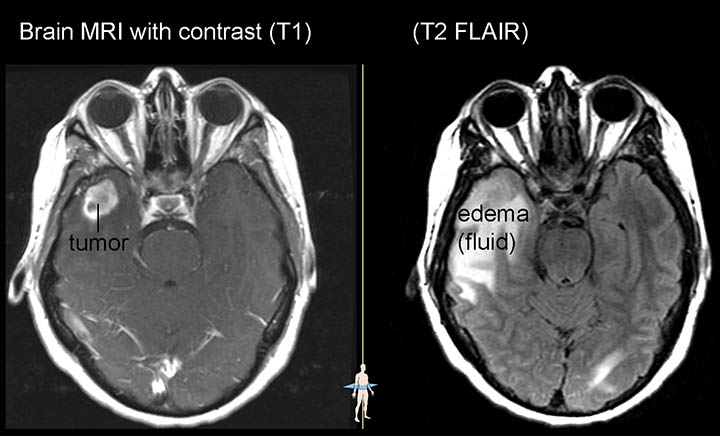
Magnetic resonance imaging (MRI) is used in lung cancer to find out whether the cancer has spread to the brain or spinal cord.7
MRI scans provide detailed pictures of areas inside the body by using radio waves and strong magnets. The energy from the radio waves is absorbed and then released in a pattern that a computer translates into images. A contrast dye is usually injected intravenously prior to the MRI to make clearer images.10
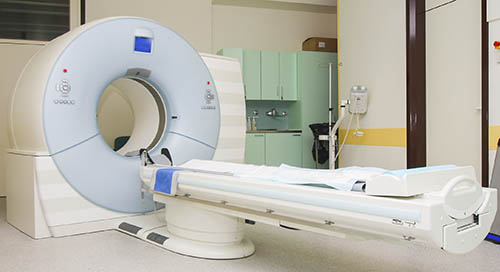
The scanner is typically a narrow tube in which a patient lies. There are special “open” MRI machines, for people who are not comfortable in a closed MRI machine, but the images are not always as clear. An MRI scan takes longer to perform than a CT scan, sometimes up to 50 minutes. Patients are given earplugs or earmuffs to help soften the loud banging noises that happen during the scans.10,11
Some Stage IIB and Stage III tumors are superior sulcus tumors, which start at the top of the lungs but can grow into the chest wall. MRIs may be used to check the extent of the growth into the spinal cord.12
Positron emission tomography (PET)
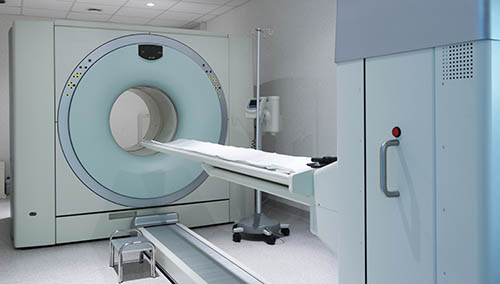
For a positron emission tomography (PET) scan, a form of radioactive sugar is given intravenously to the patient. Because cancer cells grow rapidly, they absorb more of the radioactive sugar than most healthy cells. About an hour after the injection, the patient is placed on a table in the PET scanner. The patient lies on the table for approximately 30 minutes while a special camera creates a picture of the areas in the body that absorbed the radioactive sugar.7,13
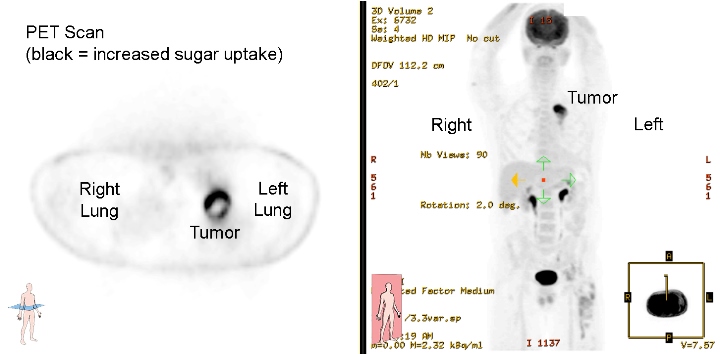
A PET scan is used to help determine whether an abnormal area on a chest X-ray or CT scan may be cancer. lt is also used to check whether cancer has spread to lymph nodes, bones, or other organs in the body. PET scans are not as useful in checking for cancer that has spread to the brain because brain cells also absorb a lot of sugar. PET scans cannot differentiate between cells that are rapidly dividing due to infection and those due to cancer; therefore, activity on a PET scan in an abnormal mass is suggestive of cancer, and biopsies are still required to be sure.2,14
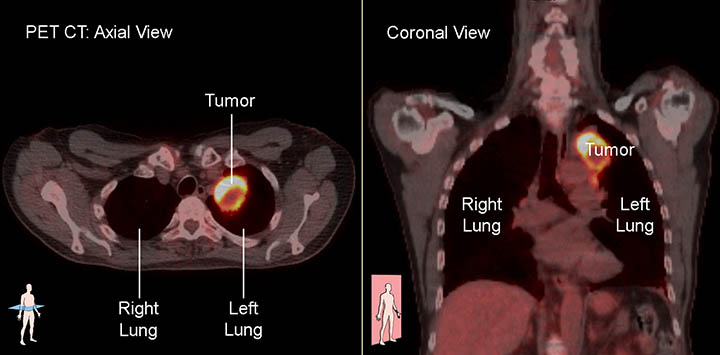
Many hospitals and radiology centers have a special scan called a PET-CT scan that is able to do a PET and a CT scan at the same time. This allows the doctor to compare areas of radioactivity on the PET scan with the more detailed appearance of that area on the CT scan.2,13
Bone scan
A bone scan is similar to a PET scan in that a small amount of a radioactive tracerA substance used in imaging procedures so that certain structures can be identified or the substance can be followed is injected into a vein. Over a couple of hours, the radioactive tracer settles in areas of the bone that have suffered injury, such as injury caused by cancer. The patient then lies on a table for 30 minutes while a camera detects the radioactivity and creates a picture of the skeleton.2,15
Since PET scans also pick up cancer in the bones, they are usually used in place of a bone scan in lung cancer.2
Updated February 12, 2024
References
- Uses of Imaging. National Cancer Institute website. http://imaging.cancer.gov/imaging_basics/cancer_imaging/uses_of_imaging.htm. Updated December 22, 2016. Accessed February 5, 2024.
- Tests for Non-Small Cell Lung Cancer. American Cancer Society website. https://www.cancer.org/cancer/non-small-cell-lung-cancer/detection-diagnosis-staging/how-diagnosed.html. Revised November 20, 2023. Accessed February 5, 2024.
- X-ray (Radiography) - Chest. RadiologyInfo.org website. www.radiologyinfo.org/en/info.cfm?pg=chestrad#common-uses. Reviewed November 01, 2022. Accessed February 5, 2024.
- NCI Dictionary of Cancer Terms. National Cancer Institute website. https://www.cancer.gov/publications/dictionaries/cancer-terms. Accessed February 5, 2024.
- Aberle DR, Adams A, et al. Reduced Lung-Cancer Mortality with Low-Dose Computed Tomographic Screening. N Engl J Med, 2011 Aug 4: 365(5); 395-409. doi: 10.1056/NEJmoa1102873. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4356534/#SD1. Published online June 29, 2011. Accessed February 5, 2024.
- Computed Tomography (CT)—Chest. RadiologyInfo.org website. www.radiologyinfo.org/en/info.cfm?pg=chestct. Reviewed November 01, 2022. Accessed February 5, 2024.
- Lung Cancer — Non-Small Cell: Diagnosis. Cancer.Net website. www.cancer.net/cancer-types/lung-cancer-non-small-cell/diagnosis. Approved December 2022. Accessed February 5, 2024.
- Computed Tomography (CT) Scans and Cancer. National Cancer Institute website. www.cancer.gov/about-cancer/diagnosis-staging/ct-scans-fact-sheet. Reviewed August 14, 2019. Accessed February 5, 2024.
- Lung Cancer Screening Guidelines. Memorial Sloan Kettering Cancer Center website. www.mskcc.org/cancer-care/types/lung/screening/screening-guidelines-lung. Copyright 2024. Accessed February 5, 2024.
- Magnetic Resonance Imaging (MRI) — Body. Radiology.Info.org website. www.radiologyinfo.org/en/info.cfm?pg=bodymr. Reviewed December 06, 2022. Accessed February 5, 2024.
- What to Expect During an MRI. Stanford Medicine Health Care website. stanfordhealthcare.org/medical-tests/m/mri/what-to-expect/during.html Copyright 2024. Accessed February 5, 2024.
- NCCN Clinical Practice Guidelines in Oncology: Non-Small Cell Lung Cancer. The National Comprehensive Care Network website. www.nccn.org/professionals/physician_gls/pdf/nscl.pdf. Version 1.2024 – December 21, 2023. Accessed February 5, 2024.
- Positron Emission Tomography-Computed Tomography (PET/CT). RadiologyInfo.org website. www.radiologyinfo.org/en/info.cfm?pg=pet. Reviewed May 1, 2023. Accessed February 5, 2024.
- Pet Scan. Penn Medicine OncoLink website. www.oncolink.org/cancer-treatment/procedures-diagnostic-tests/nuclear-medicine-tests/pet-scan. Reviewed August 22, 2022. Accessed February 5, 2024.
- Bone Scan. Cancer.Net website. https://www.cancer.net/navigating-cancer-care/diagnosing-cancer/tests-and-procedures/bone-scan. Approved October 2020. Accessed February 5, 2024.
